By Dr. David Ward
Diet is the first and most fundamental lifestyle intervention for inflammatory and autoimmune disorders to prevent the progression along the autoimmune spectrum. A Paleo-Mediterranean diet has been shown to result in improvement of overall health and a lessening of the severity of many health conditions, in particular, those with autoimmune or inflammatory components. This diet is supplemented with vitamins, minerals, fatty acids and probiotics – making it the “supplemented Paleo-Mediterranean diet”. Key dietary supplements include:
Multivitamin/multi-mineral supplementation
According to the Journal of the American Medical Association, “Most people do not consume an optimal amount of all vitamins by diet alone. …It appears prudent for all adults to take vitamin supplements”.2 Inadequate intake of nutrients is recognized as contributing to a number of chronic diseases, including “long latency” diseases that often take many years to manifest.3 Multivitamin/multimineral supplementation has been shown to improve nutritional status and reduce the risk for chronic diseases4 and provide anti-inflammatory benefits.5 The ability to safely and affordably deliver these benefits makes multimineral-multivitamin supplementation an essential component of health-promoting and disease-prevention strategies.
Vitamin D3
Vitamin D deficiency is common among patients with inflammatory and autoimmune disorders6 and supplementation has been shown to be anti-inflammatory.7 The current Recommended Dietary Allowance (RDA), defined as the average daily level of intake sufficient to meet the nutrient requirements of nearly all healthy people is 600-800 IU for adults8, however, it has been suggested that this estimate is based on an incorrect calculation.9 Accordingly, the following supplementation guidelines have been suggested6
1. Dosages of vitamin D must reflect physiologic requirements and natural production and should be in the range of 3,000–10,000 IU per day;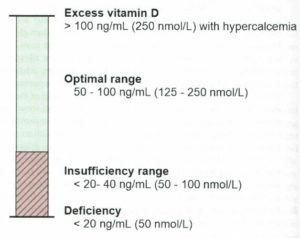
2. Vitamin D supplementation must be continued for 5-9 months for maximum benefit;
3. Supplementation should be performed with D3 rather than D2;
4. Supplements should be tested for potency;
5. Effectiveness of supplementation must include evaluation of vitamin D levels, and
6. Serum vitamin D levels must enter the optimal range.
Although rare, vitamin D toxicity and hypersensitivity can occur and consultation with a healthcare provider with appropriate education and experience for dosing recommendations and monitoring is recommended.
Balanced and complete fatty acid supplementation
There are at least five health-promoting fatty acids commonly found in the human diet10, including
· ALA, omega-3, from flaxseed oil;
· EPA, omega-3, from fish oil;
· DHA, omega-3, from fish oil and algae;
· GLA, omega-6, most concentrated in borage oil and
· oleic acid (omega-9, most concentrated in olive oil).1
Supplementing with one fatty acid can exacerbate an insufficiency of other fatty acids, and each of these fatty acids has health benefits that cannot be fully attained from supplementing a different one. A balanced supplementation approach is important because consumption of fish oil can promote a deficiency of GLA and consumption of GLA alone can reduce EPA levels while increasing levels of pro-inflammatory omega-6.11 The goal is balanced intake of all of the health-promoting fatty acids; using only one or two sources of fatty acids is not balanced and results in suboptimal improvement.1 It has been estimated that daily Paleolithic intake of omega-3 fatty acids was 7 grams per day contrasted to the average daily American intake of 1 gram per day12. Supplementation with omega-3 (EPA and DHA) and omega-6 GLA been shown to reduce the manifestations of autoimmune diseases13,14 and using combination fatty acid can ensure one is meeting metabolic needs.
Probiotics /gut microbiome modification
The microbiome is the collection of microbes (bacteria, viruses, etc.) that  live in the human habitat. Proper levels of gut bacteria promote intestinal health, support proper immune function, and encourage overall health. Imbalance in the microbiome population, called dysbiosis, can cause “leaky gut,” systemic inflammation, and a wide range of clinical problems, especially autoimmunity.15 Gut bacteria can become imbalanced by poor diets, excess stress, immunosuppressive drugs, and antibiotics, all of which are common among Americans. Restoring microbial balance by providing probiotics is an important component in the treatment of autoimmunity and systemic inflammation1 and probiotics have been shown to be therapeutically useful for the modulation of inflammatory immune disorders.16 Selection of appropriate probiotics, alone and in combination, is best done in consultation with an experienced, knowledgeable health practitioner.
live in the human habitat. Proper levels of gut bacteria promote intestinal health, support proper immune function, and encourage overall health. Imbalance in the microbiome population, called dysbiosis, can cause “leaky gut,” systemic inflammation, and a wide range of clinical problems, especially autoimmunity.15 Gut bacteria can become imbalanced by poor diets, excess stress, immunosuppressive drugs, and antibiotics, all of which are common among Americans. Restoring microbial balance by providing probiotics is an important component in the treatment of autoimmunity and systemic inflammation1 and probiotics have been shown to be therapeutically useful for the modulation of inflammatory immune disorders.16 Selection of appropriate probiotics, alone and in combination, is best done in consultation with an experienced, knowledgeable health practitioner.
Customizing the Paleo-Mediterranean diet in conjunction with vitamin-mineral supplements, vitamin D, balanced fatty acid supplementation and probiotics provides an excellent health-promoting and disease-eliminating foundation and lifestyle for many people, and is especially useful in those with chronic autoimmune and inflammatory disorders.
Dr. David Ward uses a unique blend of specialties in working with his patients. He is a licensed Doctor of Chiropractic and holds a Master of Science degree in Sport Health Science with a Sports Medicine concentration. He’s a Nationally Certified Athletic Trainer and Massage Therapist with specialty credentials as a Certified Strength and Conditioning Specialist, Performance Enhancement Specialist and Functional Medicine Practitioner. His ability to integrate musculoskeletal and metabolic medicine allows for a truly holistic approach to optimizing health and performance for a wide variety of patient populations. Dr. Ward maintains his clinical practice, Optimum Health & Performance, in the Lone Tree Runners Roost store. Dr. Ward is available for complimentary consultations for the Runners Roost community and can be reached at DocDaveWard@gmail.com. More information about Dr. Ward can be found on his website www.DocDaveWard.com.
1. Vasquez A. Revisiting the five-part nutritional wellness protocol: the supplemented Paleo-Mediterranean diet. Nutr Perspect. 2011 Jan; 34 (1):19-25.
2. Fletcher RH, Fairfield KM. Vitamins for chronic disease prevention in adults: clinical applications. JAMA 2002;287:3127-9.
3. Heaney RP. Long-latency deficiency disease: insights from calcium and vitamin D. Am J Clin Nutr 2003;78:912-9.
4. McKay DL, Perrone G, Rasmussen H, Dallal G, Hartman W, Cao G, Prior RL, Roubenoff R, Blumberg JB. The effects of a multivitamin/mineral supplement on micronutrient status, antioxidant capacity and cytokine production in healthy older adults consuming a fortified diet. J Am Coll Nutr 2000;19(5):613-21.
5. Church TS, Earnest CP, Wood KA, Kampert JB. Reduction of C-reactive protein levels through the use of a multivitamin. Am J Med 2003;115:702-7.
6. Vasquez A, Manso G, Cannell J. The clinical importance of vitamin D (cholecalciferol): a paradigm shift with implications for all healthcare providers. Altern Ther Health Med. 2004 Sep-Oct;10(5):28-36.
7. Mahon BD, Gordon SA, Cruz J, Cosman F, Cantorna MT. Cytokine profile in patients with multiple sclerosis following vitamin D supplementation. J Neuroimmunol. 2003 Jan;134(1-2):128-32.
8. Institute of Medicine, Food and Nutrition Board. Dietary Reference Intakes for Calcium and Vitamin D. Washington, DC: National Academy Press, 2010.
9. Veugelers PJ, Ekwaru JP. A statistical error in the estimation of the recommended dietary allowance for vitamin D. Nutrients. 2014 Oct 20;6(10):4472-5.
10. Vasquez A. Reducing Pain and Inflammation Naturally – Part 1: New Insights into Fatty Acid Biochemistry and the Influence of Diet. Nutr Perspect. 2004; October; 27(4): 5-14.
11. Cleland LG, Gibson RA, Neumann M, French JK. The effect of dietary fish oil supplement upon the content of dihomo-gammalinolenic acid in human plasma phospholipids. Prostaglandins Leukot Essent Fatty Acids 1990 May;40(1):9-12.
12. Cordain L, Eaton SB, Sebastian A, Mann N, Lindeberg S, Watkins BA, O’Keefe JH, Brand-Miller J. Origins and evolution of the Western diet: health implications for the 21st century. Am J Clin Nutr. 2005 Feb;81(2):341-54.
13. Simopoulos AP. Omega-3 fatty acids in inflammation and autoimmune diseases. J Am Coll Nutr. 2002 Dec;21(6):495-505.
14. Zurier RB, Rossetti RG, Jacobson EW, DeMarco DM, Liu NY, Temming JE, White BM, Laposata M. gamma-Linolenic acid treatment of rheumatoid arthritis. A randomized, placebo-controlled trial. Arthritis Rheum. 1996 Nov;39(11):1808-17.
15. Campbell AW. Autoimmunity and the Gut. Autoimmune Diseases. 2014, 152428. http://doi.org/10.1155/2014/152428
16. Kwon HK, Lee CG, So JS, Chae CS, Hwang JS, Sahoo A, Nam JH, Rhee JH, Hwang KC, Im SH. Generation of regulatory dendritic cells and CD4+Foxp3+ T cells by probiotics administration suppresses immune disorders. Proc Natl Acad Sci U S A. 2010 Feb 2;107(5):2159-64.















Recent Comments